Gabriella Captur, MD PhD, MRCP, MSc†; Chinwe Obianyo MD*, Rebecca Hughes*†, Charlotte Manisty*†, James Sneddon, MD†; James C Moon, MBBS, MRCP*†
*Institute of Cardiovascular Science, University College London, London, UK
†CMR Unit, The Barts Heart Centre, St Bartholomew’s Hospital, London, UK
Clinical History
A 64-year old Caucasian lady was seen at the rapid access chest pain clinic with a 6-month history of atypical chest pain. Her risk factors for cardiovascular disease were smoking, hypertension and familial risk. She was referred for coronary angiography that revealed moderate right coronary artery/posterior descending artery stenosis while left ventriculography suggested an unusual cardiac orientation with a laterally displaced and vertically oriented heart. She was referred to us for stress perfusion cardiovascular magnetic resonance (CMR) imaging.
CMR Findings
Cardiovascular magnetic resonance (CMR, Movies 1-7) revealed congenital partial left sided absence of the pericardium.
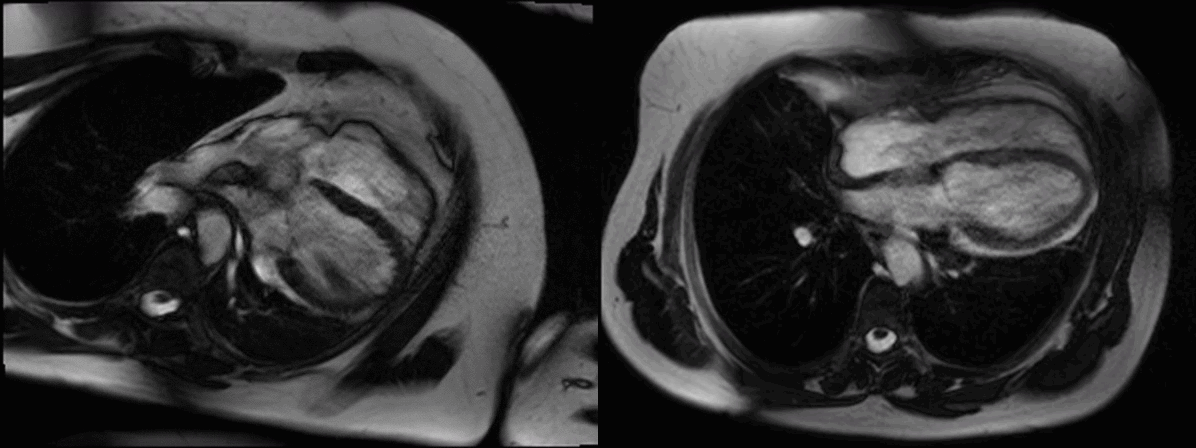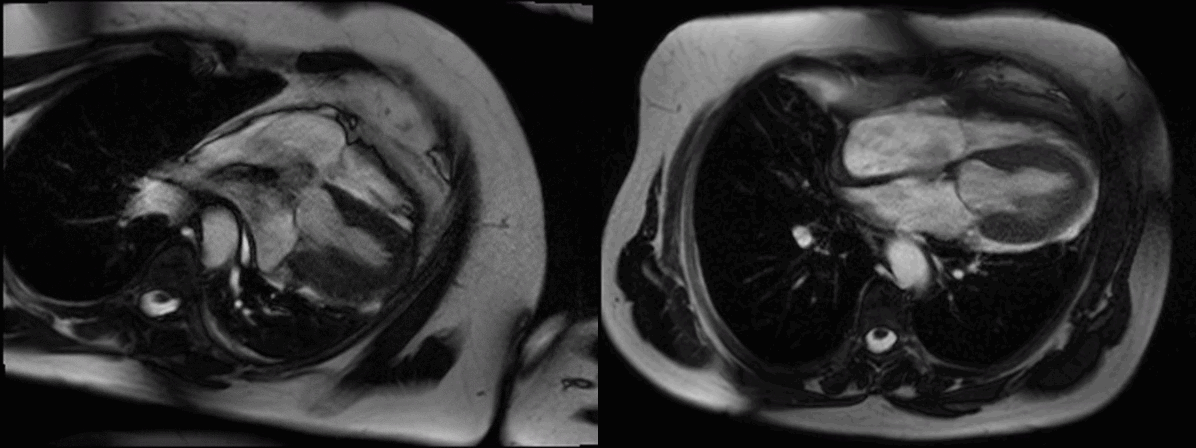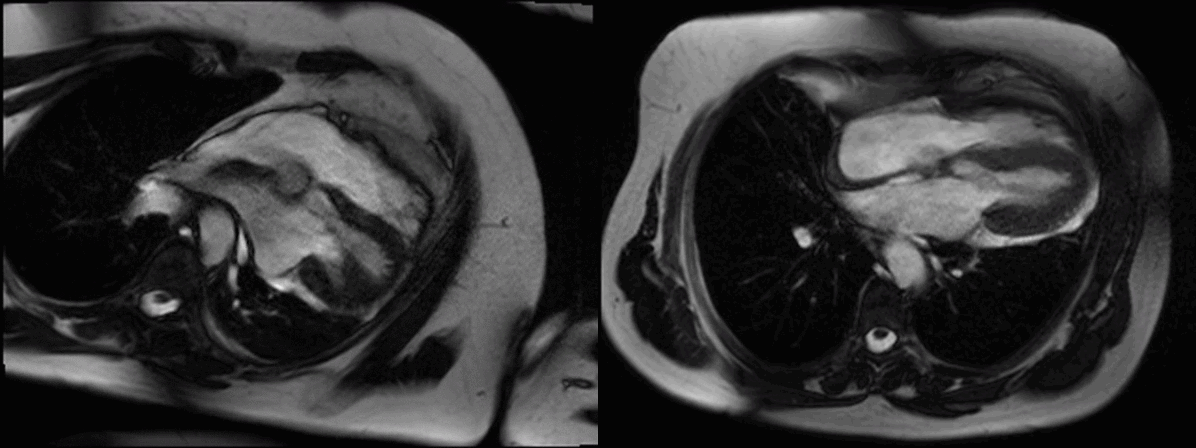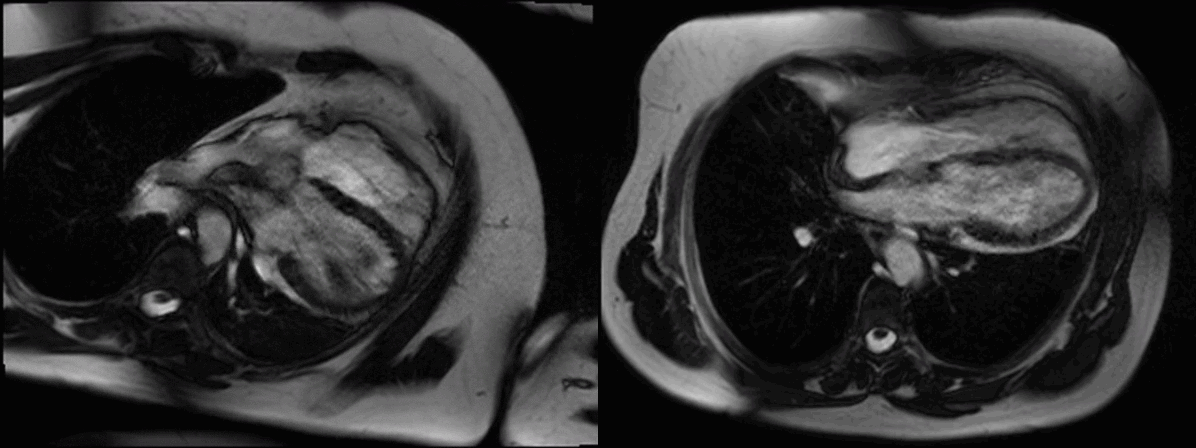
Movie 1 (4 chamber supine) and Movie 2 (4 chamber prone)
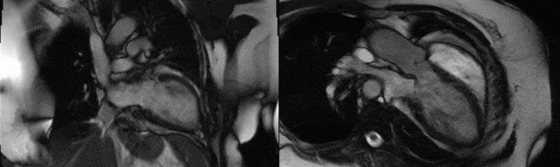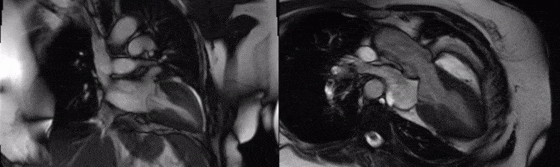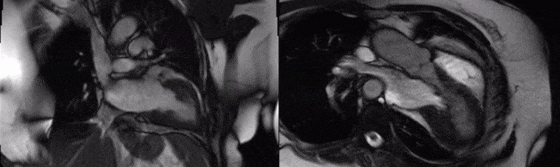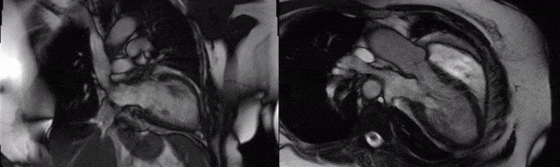
Movie 3 (2 chamber) and Movie 4 (3 chamber)
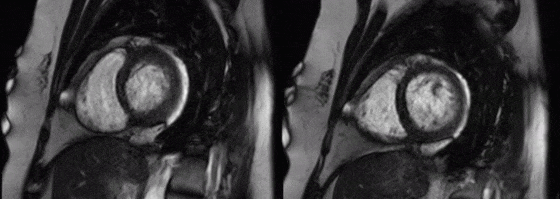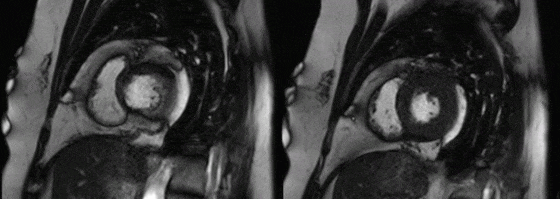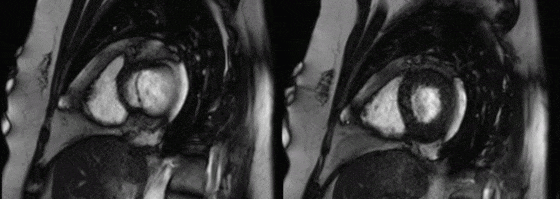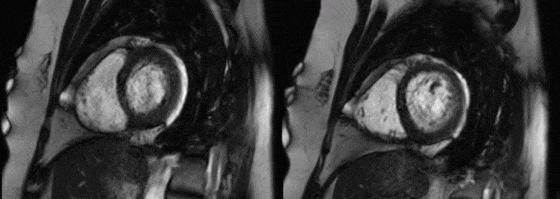
Movies 4 and 5: basal mid short axis
In the supine position (Figure A, axial breath-held T1-weighted turbo-spin echo) there was levo-positioning of the heart and posterior left ventricular (LV) displacement with the apex pointing towards the posterior axillary line (white asterix) and rightward displacement of the descending thoracic aorta. We rescanned the patient in the prone position and demonstrated a novel, potentially useful CMR sign in suspected cases of congenital absence of the pericardium: the heart ‘flops’ ventrally (Figure B, black asterix) highlighting the great mobility of the heart with a pericardial defect.
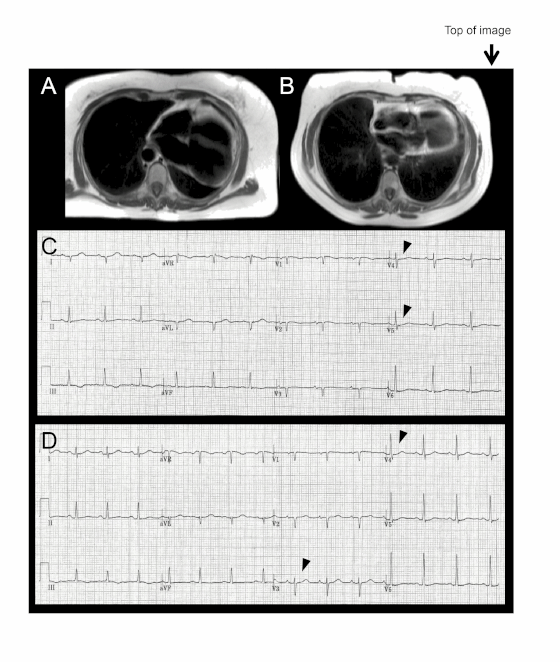
Electrocardiography (ECG) in this supine position (Figure C) showed right axis deviation, poor R wave progression and leftward displacement of the transition zone (arrowheads) in the precordial leads (the normal transition zone is generally between V3 and V4). In the prone position the heart’s ventral ‘flop’ normalizes the transition zone across the precordial ECG leads (Figure D, arrowheads)
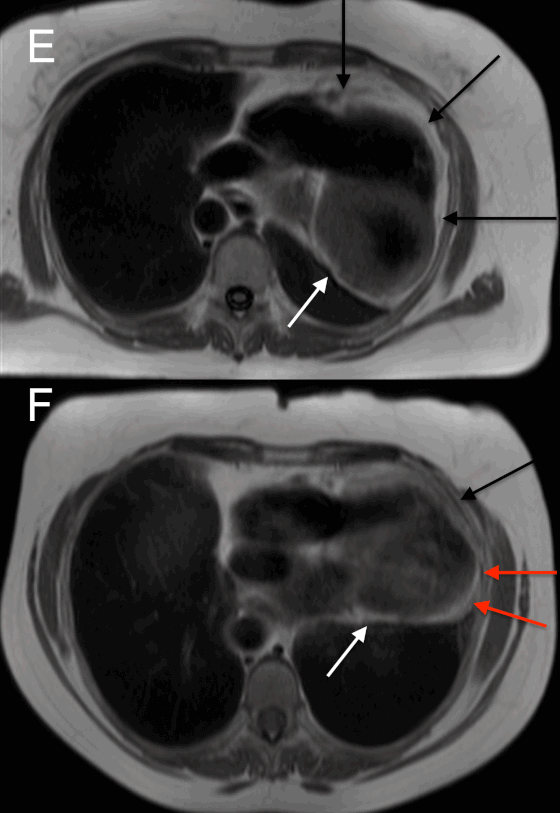
Other CMR signs convinced us that this was a case of partial as opposed to complete left sided absence of the pericardium. Firstly, axial T1-weighted imaging in the supine (Figure E) and prone positions (Figure F), showed the presence of the pericardium overlying the right ventricle (black arrows point to a dark stripe sandwiched between bright epicardial and pericardial fat). No pericardium was visible overlying the LV in the supine position but in the prone position, a pericardial stripe could be seen over the LV apex and terminating posteriorly (red arrowheads) thus suggesting partial as opposed to complete absence. A thin rim of epicardial fat was visible around the LV in both views (white arrows).
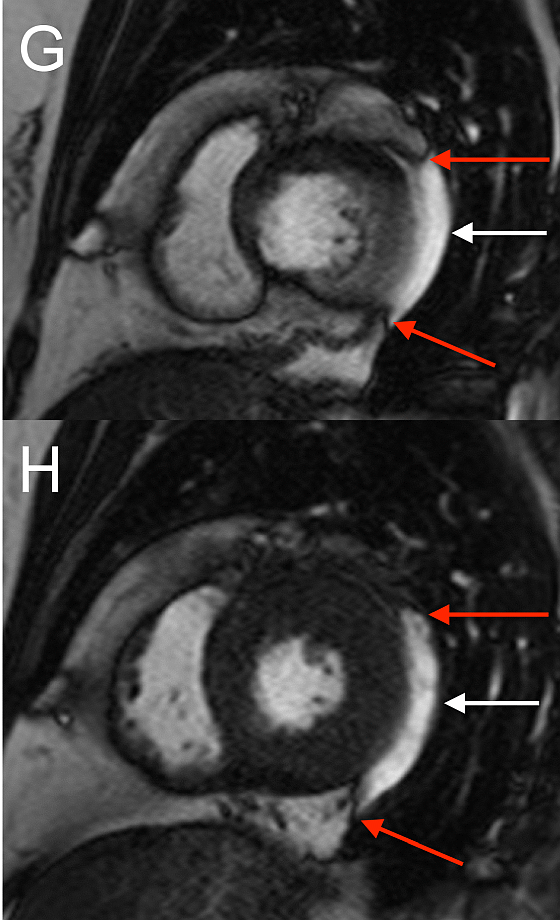
On LV short axis cines (Figures G and H), the pericardium was visible only overlying anterior and inferior portions of the LV, and was absent over the lateral wall, indicating a congenital partial left absence of pericardium(1).
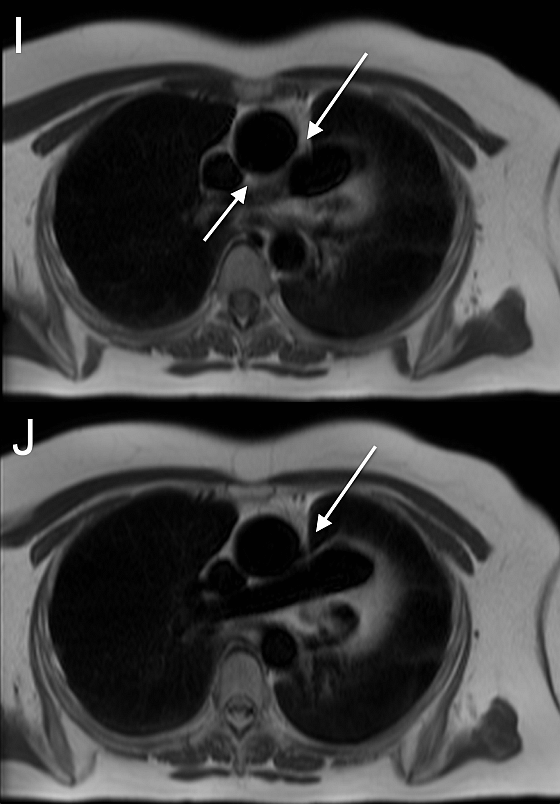
CMR also demonstrated the absence of anterior and posterior superior pericardial recesses around the ascending aorta at the level of the pulmonary artery bifurcation (Figure I, white arrows). Lung tissue was insinuated between the aorta and pulmonary artery, indicating the absence of pericardium at this level (Figure J). Left and right ventricular function were within normal limits, as were cavity sizes. There was no inducible ischaemia during adenosine stress perfusion and no previous infarction or scarring on late gadolinium enhancement imaging. No coronary artery anomalies or defects of the atrial or ventricular septa were noted.
The patient was commenced on aspirin and statin for primary prevention given the moderate coronary artery disease identified. No specific management was required for the congenital partial absence of pericardium.
Conclusion
Here we present a quick and simple CMR sign–the ventral cardiac ‘flop’–that may be useful in confirming a suspected case of congenital absence of the pericardium at the time of CMR scanning.
Perspective
Congenital absence of the pericardium(2) is a rare cardiac condition, most often asymptomatic, thought to arise from premature atrophy of the common cardiac veins supplying the pleuropericardial membranes(3, 4) resulting in partial or complete, pericardial agenesis. It may also be associated with other congenital heart defects (this patient had none). It may be associated with other congenital heart defects although in our patient it was an isolated finding. Historically it has been incidentally diagnosed post-mortem or intraoperatively while attempted repair associated defects like diaphragmatic hernias(5).
Echocardiography may point to the diagnosis on the basis of a displaced apex and abnormal septal motion although echocardiography may be technically challenging in these patients because of unusual heart orientation within the chest cavity and significant cardiac motion(1). Computed tomography, like CMR(6), is capable of showing the classical interposition of left lung tissue in between the great vessels plus loss of linear continuity of the pericardium. Pericardial evaluation can be quite challenging in patients with a prominent pericardial fat layer. Even using multiple imaging modalities and searching for this key set of diagnostic cues, unequivocal diagnostic certainty is still not achieved in a proportion of patients with congenital absence of the pericardium, highlighting the added clinical utility of the ventral cardiac ‘flop’ sign we describe here.
Eliciting this additional CMR sign (the ventral cardiac ‘flop’) by prone position scanning, may be useful in corroborating diagnostic certainty of congenital absence of the pericardium at the time of CMR scanning. This may help technicians scanning the patient, and doctors on site supervising the scan, more robustly identify cases of absent pericardium, allowing them to perform targeted acquisitions before the patient leaves the department. Prone position scanning is useful but not mandatory for diagnosing absent pericardium. Not mandatory, in so far as the diagnosis can often be made on the basis of the other imaging signs present.
Here we present an additional CMR sign (the ventral cardiac ‘flop’) that may be useful in corroborating diagnostic certainty of congenital absence of the pericardium, at the time of CMR scanning.
Click here to view the entire case on CloudCMR
Case was prepared by Associate Editor: Dr. Sylvia Chen
References
1. Brulotte S, Roy L, Larose E. Congenital absence of the pericardium presenting as acute myocardial necrosis. Can. J. Cardiol. 2007;23:909–912.
2. Kim H-J, Cho Y-S, Cho G-Y, Choi S Il. Congenital absence of the pericardium. J. Cardiovasc. Ultrasound 2014;22:36–39.
3. Verde F, Johnson PT, Jha S, Fishman EK, Zimmerman SL. Congenital absence of the pericardium and its mimics. J. Cardiovasc. Comput. Tomogr. 2013;7:11–7.
4. Broadbent JC, Callahan J a, Kincaid OW, Ellis FH. Congenital deficiency of the pericardium. Dis. Chest 1966;50:237–44.
5. Shimada Y, Yoshida J, Aokage K, Hishida T, Nishimura M, Nagai K. Complete left-sided pericardial defect in a lung cancer patient undergoing pneumonectomy without closure of the defect. Ann. Thorac. Cardiovasc. Surg. 2011;17:67–70.
6. Leong DP, Chakrabarty A, Brooks AG, Bridgman C, Selvanayagam JB. Cardiac Magnetic Resonance Findings in Congenitally Absent Pericardium. J. Am. Coll. Cardiol. 2009;54:2459.







