Afiachukwu Onuegbu MD, Jina Chung MD
Division of Cardiology, Harbor UCLA Medical Center
Case Published in the Journal of Cardiovascular Magnetic Resonance: Click here for the link
Click here for PubMed Reference to Cite this Case
Clinical History:
A 20 year old man with past medical history of spontaneous left pneumothorax presented with atypical chest pain, palpitations and lightheadedness. His transthoracic echocardiogram (TTE) showed normal left ventricle ejection fraction (LVEF), with prominent right ventricle (RV) trabeculations with mildly reduced right ventricular function, and right ventricular dilation (Movie A). Subsequent bubble study (video not shown) done with agitated saline injection in the left antebrachial vein resulted in early opacification of a dilated coronary sinus before the right atrium, which was suggestive of persistent left sided superior vena cava (PLSVC). When agitated saline was injected into the right antebrachial vein (video now shown), the right atrium opacified before the coronary sinus confirming a normal right superior vena cava. The RV findings raised a concern for arrhythmogenic right ventricular dysplasia (ARVD) or RV non-compaction. Cardiac MRI was ordered to further evaluate the RV.
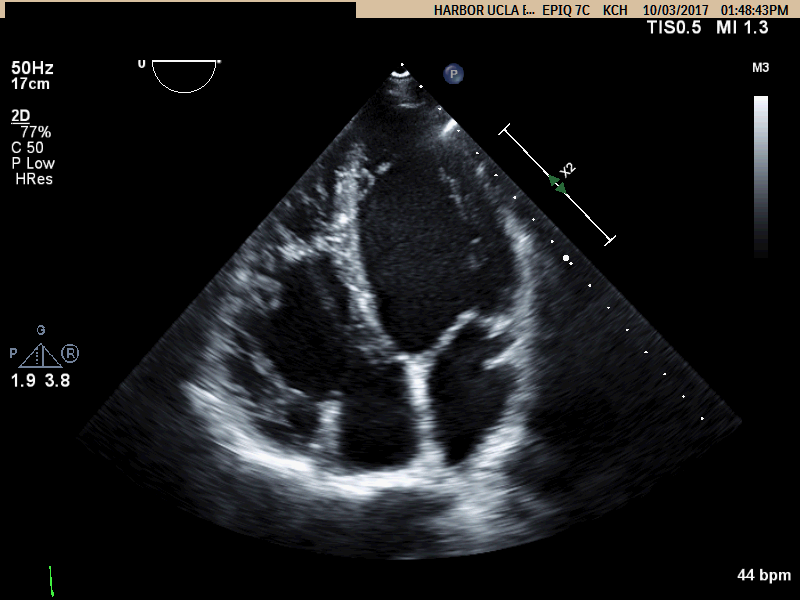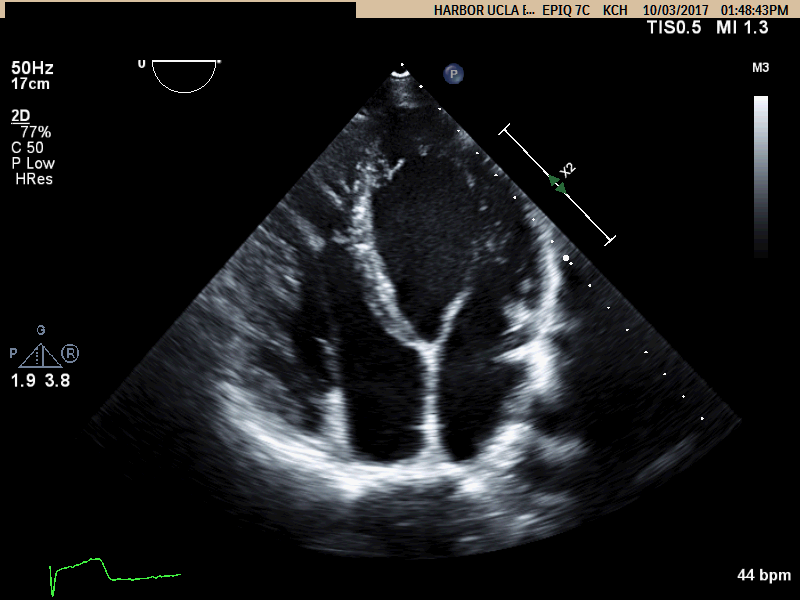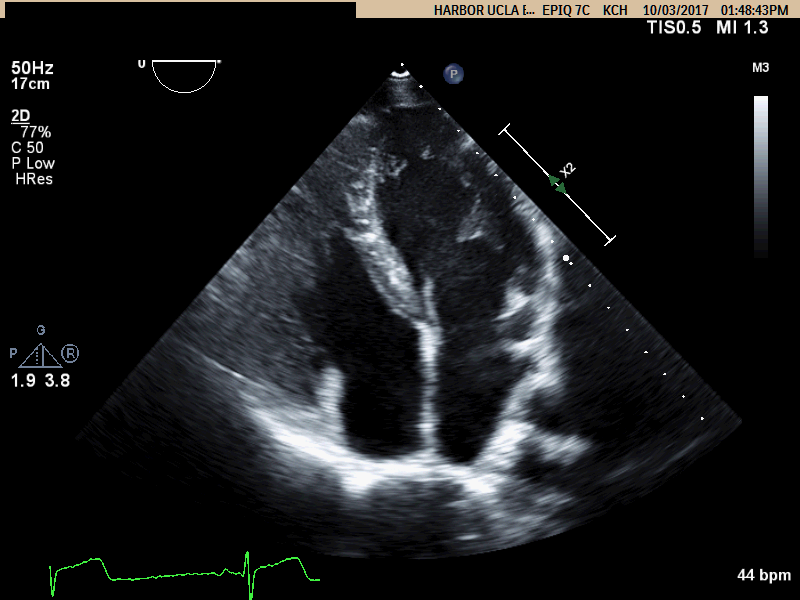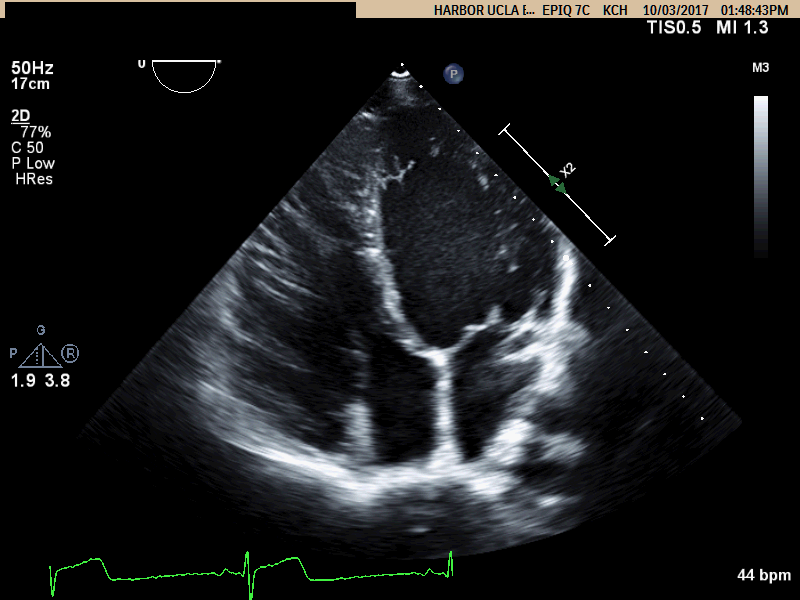
Movie A: Apical 4 Chamber view showing RV dilation
CMR Findings: A cardiac MRI and 3-dimensional time-resolved magnetic resonance angiography (3D MRA) showed normal left and right ventricular systolic function and wall thickness with mild left ventricle (LV) dilation and RV size at upper limits of normal (LVEF 61%, RVEF 51%, LV end diastolic volume index 123.5 ml/m2, RV end diastolic volume index 103ml/m2). No right ventricular regional wall motion abnormalities or dyskinesis were present. T1, T2 weighted images pre and post contrast revealed no fatty infiltration or fibrosis of RV. Hence, cardiac MRI did not meet the criteria for ARVD or RV non-compaction. Instead, cardiac MRI and 3D MRA identified two venous anomalies: A PLSVC draining into the right atrium via the coronary sinus and the azygos continuation of the inferior vena cava (IVC) with an absent hepatic segment of IVC. (Movies C, D, E). Also seen is the hemiazygos vein draining into the PLSVC.
Movies B, C, and D show the patient’s time resolved 3D cardiac MRA in the coronal, axial and sagittal planes. A persistent left sided superior vena cava is readily identified and seen draining into the coronary sinus, which drains into the right atrium. The azygous continuation of the inferior vena cava is appreciated particularly well in Movie C but can also be seen in Movie B. The MR angiograms demonstrate the azygos continuation of IVC coursing along the right side of the descending aorta and then draining into the right SVC at the right paratracheal space. Also seen is the hemiazygos vein draining into the PLSVC.
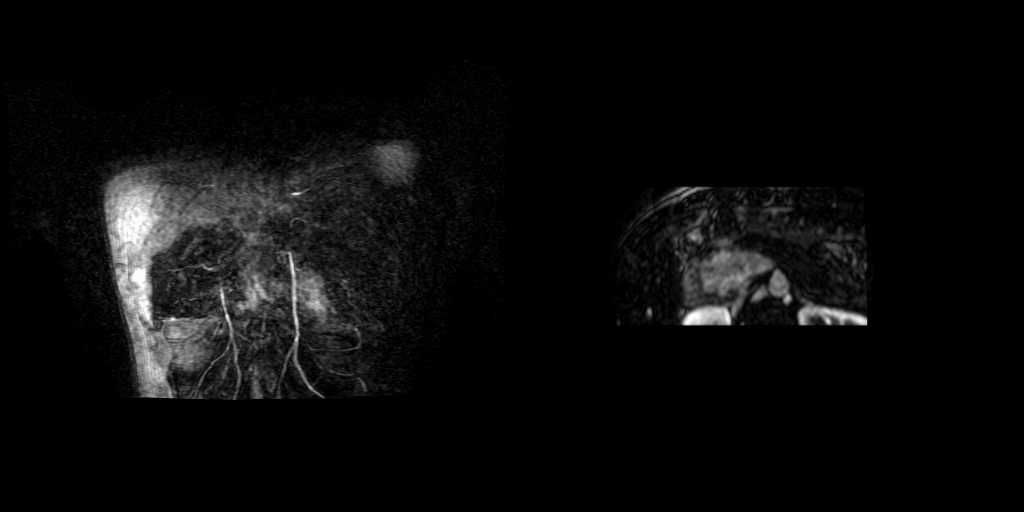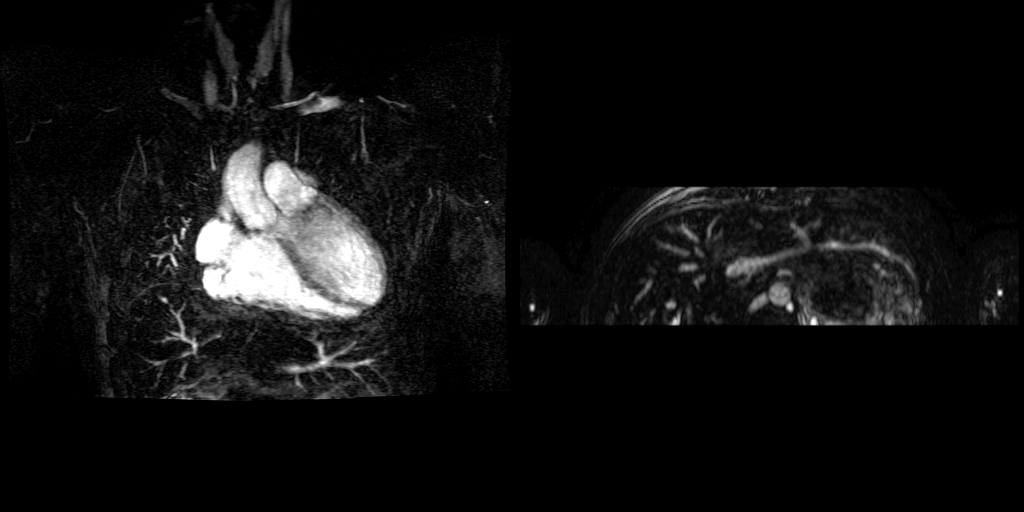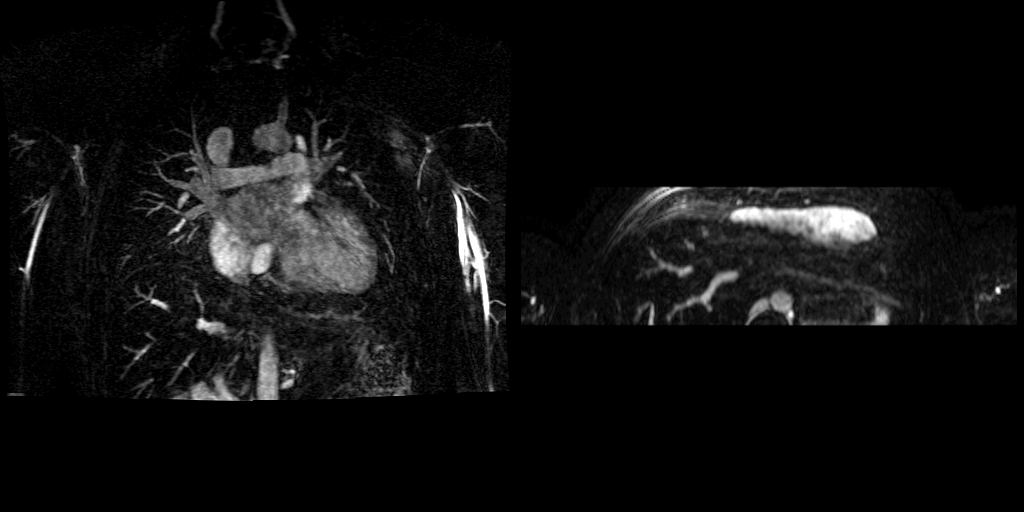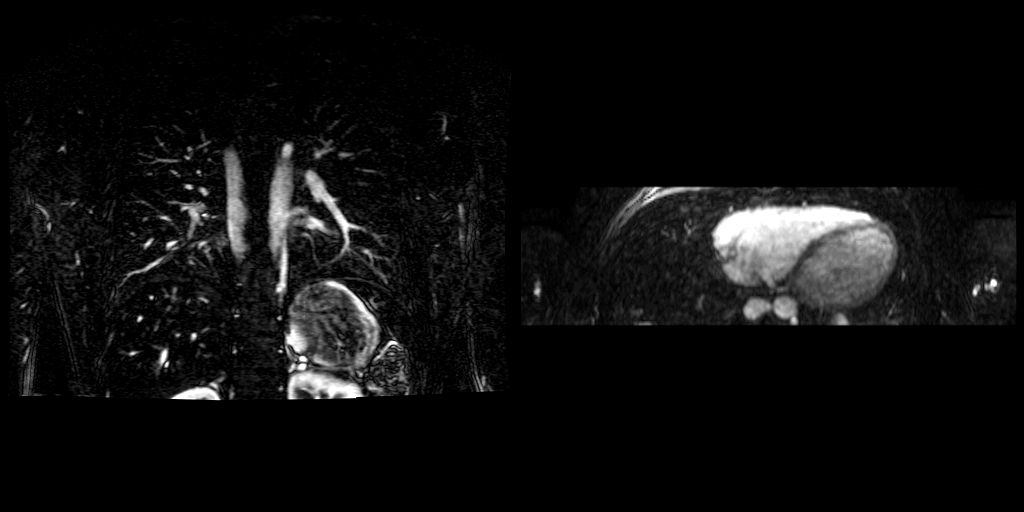
Movie B Movie C
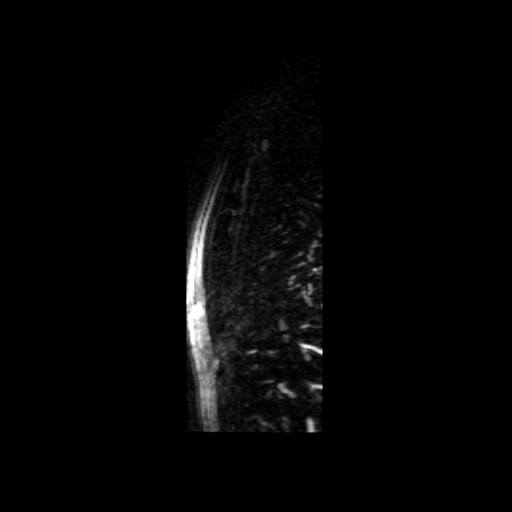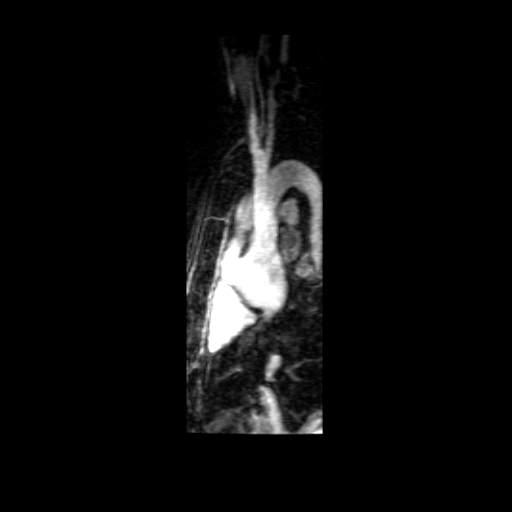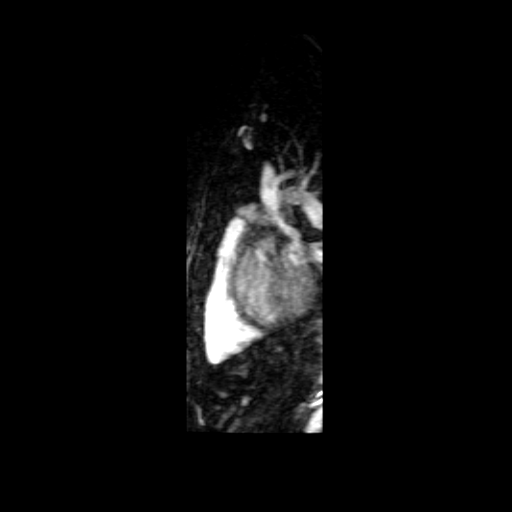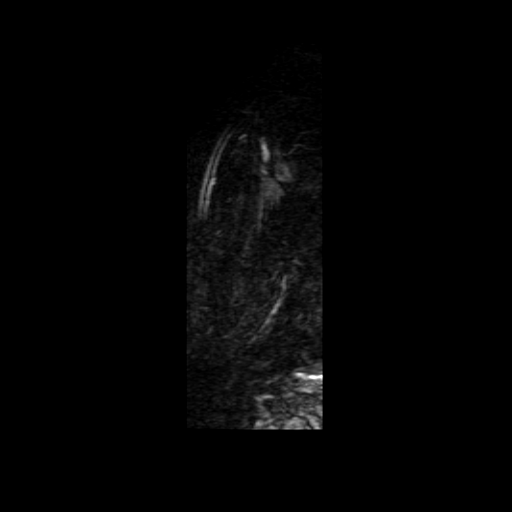
Movie D
Conclusion: In view of the patient’s young age and abnormal RV findings on TTE, ARVD was considered as a possible etiology of his clinical presentation. As a gold standard for RV assessment, the cardiac MRI and MRA study clarified that the patient had a normal RV size, normal RV function and tissue characteristics and also revealed two major anomalous venous connections. This case highlights the versatility of cardiac MRI and MRA in the evaluation patients with suspected RV or congenital abnormality.
Perspective: Azygos continuation of the IVC with absence of the hepatic segment of IVC is a rare finding with a prevalence of 0.6% among patients with congenital heart defects. [1] It has been shown to be sometimes associated with other congenital anomalies like heterotaxy syndromes, cor biloculare, PLSVC, anomalous pulmonary venous return, double outlet right ventricle, large atrial septal defect and pulmonary atresia. [1] The embryonic event is theorized to be failure of the union of the right subcardinal and hepatic anastomosis, with resulting atrophy of the right subcardinal vein [1].
The renal portion of the IVC receives blood from both kidneys and passes posterior to the diaphragmatic crura to enter the thorax as the azygos vein. The azygos vein joins the superior vena cava at the normal location in the right paratracheal space through a dilated azygos arch [2]. Since the advent of multimodality imaging this entity is now being increasingly recognized in otherwise asymptomatic patients [3]. It is important to recognize the enlarged azygos vein at the confluence with the superior vena cava and in the retrocrural space to avoid misdiagnosis as a right-sided paratracheal mass or retrocrural adenopathy [4]. Preoperative knowledge of the anatomy may be important in planning cardiopulmonary bypass and to avoid difficulties in cardiac catheterization.
Click here to review the case on CloudCMR
Case prepared by:
Ashish Aneja MD FSCMR FASE FACC
Associate Editor, SCMR Case of the Week
MetroHealth Medical Center, Case Western Reserve University
Cleveland, Ohio







