Andrew A. Pavlina, MD1, Kaushik Chagarlamudi2, Sangita Kapur, MD1
- University of Cincinnati Department of Radiology, Cincinnati, OH, USA
- Northeastern Ohio Medical University, Rootstown, OH, USA
Clinical History:
A 54-year-old male with a history of heart failure and coronary artery disease and recent LAD stenting presented with chest pain and shortness of breath. He was noted to have a fever to 101.5 ° F and decreased breath sounds in the left lung base. On initial laboratory workup he was noted to have normal troponin levels but an elevated white count. His EKG demonstrated pathologic Q waves consistent with a remote anteroseptal and inferior infarct [Image 1].
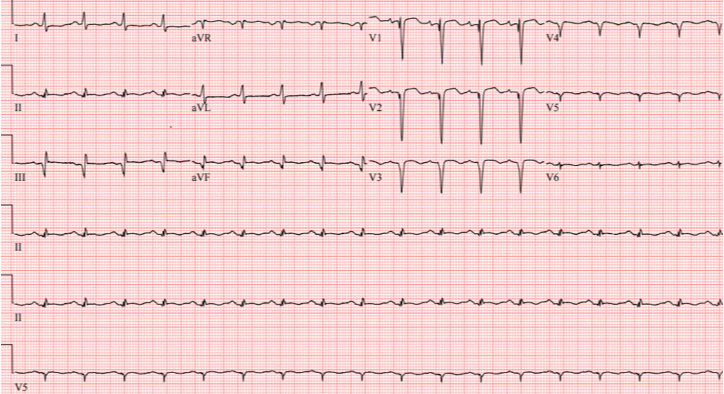
Image 1. Initial EKG demonstrating findings compatible with prior anteroseptal and inferior infarct.
Initial imaging with a chest radiograph demonstrated a moderate sized left pleural effusion which was found to represent empyema after chest tube drainage. Subsequent contrast-enhanced chest CT showed a left pleural effusion, mediastinal lymphadenopathy, and a round area of hypo-enhancement involving the cardiac apex with likely pleural extension [Image 2].
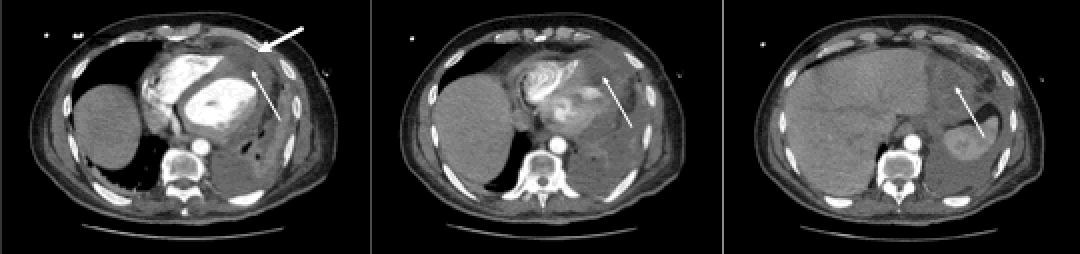
Image 2. Axial Contrast Enhanced CT images demonstrated hypo enhancement along the cardiac apex (arrows) with a possible small tract leading to the pleural space (bold arrow). Additionally there is pericardial thickening and effusion, pleural effusion, and left lower lobe consolidation.
Initial differential diagnosis considerations included a necrotic cardiac mass or myocardial necrosis with rupture. Cardiac MRI was performed to further aid in diagnosis.
Cardiac MRI Findings:
Cardiac MRI with and without contrast was performed on a 1.5 T MRI (GE Healthcare). Steady State Free Precession (SSFP) cine imaging demonstrated a 6 x 6.4 x 5.9 cm loculated heterogeneous and T2 hyperintense collection adjacent to left ventricular apex and interventricular septum consistent with contained left ventricular apical rupture with pseudoaneurysm formation [Movie 1].
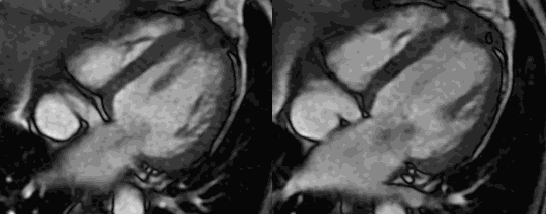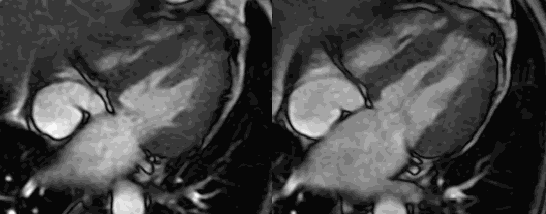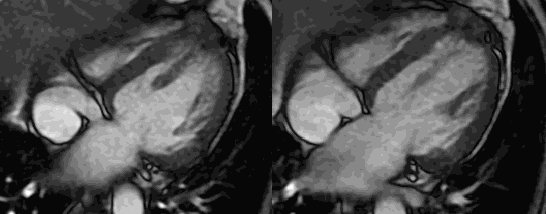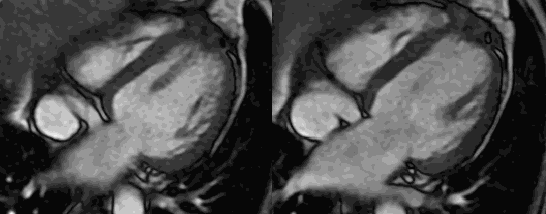
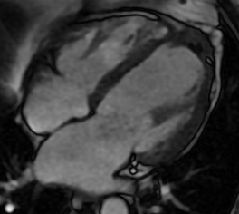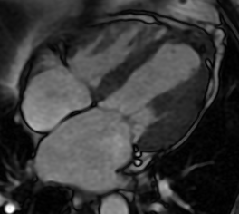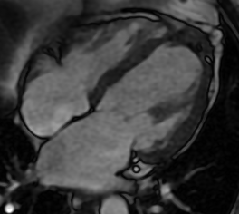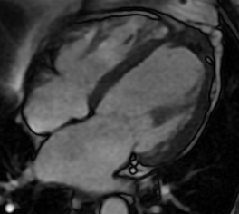
There was a left pleural effusion which had apparent communication with the pericardial space. There was edema and dyskinesis of the apical septum, anterior wall and true apex. Late gadolinium enhanced (LGE) images showed late transmural enhancement involving the LAD territory consistent with prior infarct and non-viability. [Image 3]. The pericardium was thickened with late enhancement consistent with pericarditis [Image 3].
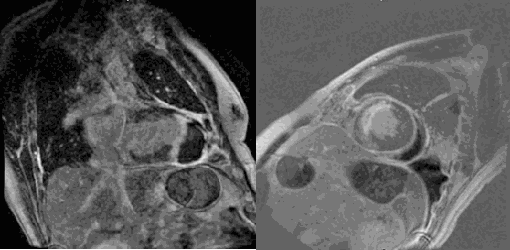
Image 3. Phase sensitive late gadolinium enhancement two chamber (left) and short axis at the mid-ventricular level (right) demonstrating transmural LGE in the left anterior descending coronary artery distribution, apical pseudoaneurysm, in addition to pericardial thickening and enhancement.
Conclusion:
In this case Cardiac MRI was essential to diagnose an apical cardiac rupture with left ventricular pseudoaneurysm formation and to exclude a cardiac mass. The patient subsequently underwent left pleural decortication and repair of the pseuoaneurysm with an extracellular matrix xenograft. The pseudoaneurysm contained purulent material which grew the same organism (Bacteroides Fragilis) as the pleural fluid collection. The patient was discharged on postoperative day 11 and his symptoms were well controlled. A follow-up cardiac MRI demonstrated postsurgical changes from apical repair without evidence of recurrent pseudoaneurysm [Image 4].
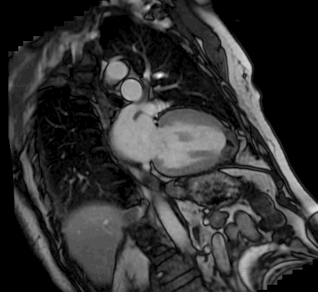
Image 4. Post-operative CMR cine demonstrating surgical changes with no recurrent pseudoaneurysm after four years.
Perspective:
Risk factors for left ventricular pseudoaneurysm include myocardial infarction, infection, prior cardiac surgery, or trauma [1,2]. In the setting of infarction, a pseudoaneurysm forms when a ventricular free wall rupture is contained by thrombus or fibrous tissue. Ventricular free wall rupture without pseudoaneurysm formation occurs after approximately 2-4% of myocardial infarctions and typically presents with rapid hemodynamic collapse within 24 hours to 1 week. When a pseudoaneurysm does form, on the other hand, it can be clinically undetectable or have a delayed presentation with signs of congestive heart failure, arrhythmia, or embolism [1,3,4]. The biggest concern with left ventricular pseudoaneurysm is the risk of rupture which occurs in an estimated 30-45% of patients and thus necessitates surgical repair [2,3].
In this case, the left ventricular pseudoaneurysm was further complicated by an anaerobic infection which involved the pericardial and pleural spaces. While the exact source of the infection is unknown, it is felt likely to be secondary to Bacteroides bacteremia. Similar cases of cardiac infection or abscess in the absence of endocarditis have been reported in patients who have seeded a thrombus, remote infarct, or ventricular aneurysm [5,6]
As was true in this case, cardiac MRI is an extremely useful tool in the diagnosis of ventricular pseudoaneurysm. Firstly, it is noninvasive and does not expose the patient to ionizing radiation. It allows for the visualization of the heart in any plane which may be difficult to achieve with traditional echocardiography [2]. Additionally, it has high spatial resolution and allows for simultaneous tissue characterization and functional evaluation [7]. This is particularly useful when trying to distinguish pseudoaneurysm, which requires more urgent surgical evaluation, from true cardiac aneurysm or other type of ventricular outpouching. Dynamic MRI imaging allows for the direct visualization of a communication between the ventricle and pseudoaneurysm and can be used to assess or measure cardiac wall motion. Finally, MRI is useful for demonstrating various enhancement patterns such as late myocardial enhancement seen with prior myocardial infarction or late pericardial enhancement which can be associated with ventricular pseudoaneurysm [7].
References
- Mahilmaran A, Nayar PG, Sheshadri M, et al: Left ventricular pseudoaneurysm: caused by coronary spasm, myocardial Infarction, and myocardial rupture. Texas Heart Institute Journal 2002; 29(2):122-125.
- Bisoyi S, Dash AK, Nayak D, et al: Left ventricular pseudoaneurysm versus aneurysm a diagnosis dilemma. Annals of Cardiac Anesthesia 2016; 19(1): 169-172.
- Mujanovic E, Bergsland J, Avdic S, et al: Surgical treatment of left ventricular pseudoaneurysm. Medical Archives 2014; 68(3):215-217.
- Amir O, Smith R, Nishikawa A, et al: Left ventricular free wall rupture in acute myocardial infarction: a case report and literature review. Texas Heart Institute Journal 2005; 32(3):424-426.
- Nand N, Singla SK, Magu S: Cardiac abscess with ventricular aneurysm secondary to old myocardial infarction. Journal of the Association of Physicians of India 2017; 65(5): 95-96.
- Starkey IR, Kaplan DK, Thorpe JA: Staphylococcal infection of a left ventricular aneurysm. Thorax 1986; 41:154-155.
- Sharma A, Kumar S: Overview of left ventricular outpouchings on cardiac magnetic resonance imaging. Cardiovascular Diagnosis and Therapy 2015; 5(6): 464-470.
Click here for complete cardiac MRI images on CloudCMR
Case prepared by: Eddie Hulten, MD; Associate Editor, Case of the Week







